Treatment Abroad – Find Verified Clinics, Reviews & Prices
Treatment Abroad made simple by A-Medical. Explore top clinics worldwide and start your journey toward better health today
We make healthcare abroad
simple, transparent, and fully guided from start to finish
Submit Your Request
Tell us about your treatment needs. We carefully review your case and match you with the most suitable hospitals and doctors.
Get Official Price Quotes
We provide verified treatment offers and proformas directly from hospitals — no middlemen, full transparency.
Connect with Doctors
We arrange direct calls or video consultations with hospitals and doctors so you can discuss your treatment plan confidently.
Confirm & Start Treatment
Once you accept the treatment plan, we schedule your hospital appointment and support you throughout your medical journey.
Clinics
Discover our network of world-class medical facilities offering comprehensive healthcare services
Why Choose Us
With us, you are in safe hands. We focus on quality, transparency, and patient-first care. Here’s what sets us apart
Only Accredited Hospitals
We partner exclusively with internationally accredited and top-ranked hospitals.
Direct & Transparent Payments
You pay directly at the hospital, with no hidden fees.
Free Direct Call & Video Consultation
Speak with our experts and doctors before making any decisions.
Best Doctor & Hospital Match
We carefully select the most suitable specialist and clinic for your treatment needs.
Worldwide Hospital Network
Access to a vast global network across 90+ countries.
More Affordable Pricing
We negotiate better prices from hospitals than you would get by contacting them directly.
Medical Conditions
Explore our comprehensive coverage of medical conditions and find the right treatment options
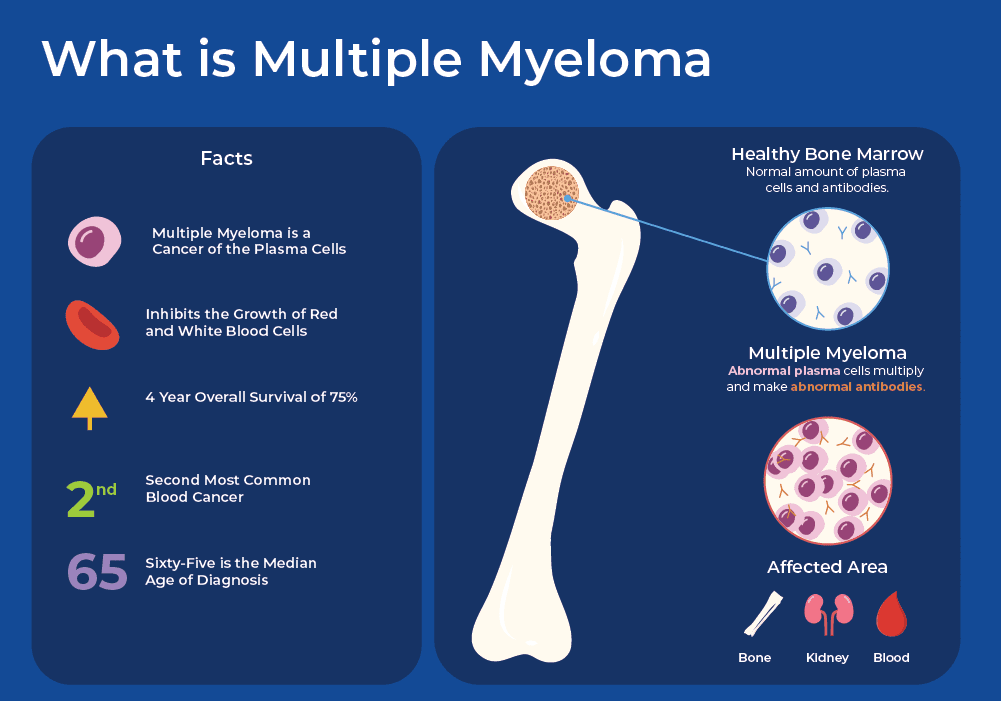
Multiple Myeloma
A type of cancer of plasma cells that develops in the bone marrow.

Glioma
A glioma is a type of brain tumor that develops in the central nervous system and originates from glial cells. These cells play a vital role in maintaining the health and function of nerve cells. When genetic mutations occur in glial cells, uncontrolled growth can lead to tumor formation. Gliomas can develop in different parts of the brain and spinal cord. The most common locations include the cerebral hemispheres, brainstem, cerebellum, and spinal cord. The tumor’s size, location, and growth rate vary significantly from one patient to another. Although gliomas are relatively rare compared with other cancers, some subtypes are more common than others. Understanding glioma types, symptoms, diagnosis, and treatment options is essential for early detection and effective care. Specialized treatment is available at leading centers such as Sheba Medical Center. Glioma Types Glioma is an umbrella term that includes several subtypes, classified based on the type of glial cell involved and the tumor’s location. Astrocytoma Astrocytomas arise from astrocytes, star-shaped glial cells that support and protect neurons. These tumors often infiltrate healthy brain tissue, making high-grade astrocytomas difficult to remove completely. Grades: Grade 1: Pilocytic astrocytoma, SEGA, pleomorphic xanthoastrocytoma Grade 2: Diffuse astrocytoma Grade 3: Anaplastic astrocytoma Grade 4: Glioblastoma Most diagnosed gliomas are astrocytomas, ranging from low-grade to highly aggressive forms. Brainstem Glioma Brainstem gliomas develop in the brainstem, a region that controls vital functions such as breathing and heart rate. Because of their location, surgery is often not possible. Types: Focal brainstem gliomas: Slow-growing, localized, less aggressive Diffuse intrinsic pontine glioma (DIPG): Rapidly growing, highly aggressive, infiltrates surrounding tissue Ependymoma Ependymomas originate from ependymal cells, which line the ventricles of the brain and the central canal of the spinal cord. Grades: Grade 1–2: Low-grade, often found in the spinal cord Grade 3: High-grade, more common in the brain Mixed Glioma Mixed gliomas contain more than one type of glial cell. Their behavior and aggressiveness depend on the specific cell combination and tumor grade. Oligodendroglioma Oligodendrogliomas arise from oligodendrocytes, cells that insulate nerve fibers. Grades: Grade 2: Slow-growing, low-grade Grade 3 (Anaplastic): Fast-growing, aggressive Optic Pathway Glioma Optic gliomas develop along the optic nerve, optic chiasm, or hypothalamus, often affecting vision. Stages: Stage 1: Optic nerve involvement Stage 2: Optic chiasm involvement Stage 3: Hypothalamic involvement Glioma Symptoms Symptoms depend on tumor location and size. Common signs include: Persistent or worsening headaches Difficulty with balance and walking Vision problems Nausea and vomiting Sudden seizures Confusion or memory problems Personality or behavioral changes Speech difficulties Unexplained weight changes Symptoms vary widely, and not all patients experience the same signs. Risk Factors Known factors associated with a higher risk of glioma include: Genetic conditions: Neurofibromatosis type 1, Turcot syndrome, Li-Fraumeni syndrome Family history: Rare, but reported in some families Previous exposure to ionizing radiation, especially childhood radiotherapy Age: More common in children aged 5–8 and adults aged 45–65 Glioma Diagnosis Diagnosis involves multiple steps: Physical exam and medical history Neurological examination CT scan for structural imaging MRI for detailed tumor visualization Biopsy to identify tumor type and grade Lumbar puncture (in select cases) Molecular testing to guide personalized treatment Glioma Grading Gliomas are graded from 1 to 4, based on how abnormal the tumor cells appear and how fast they grow. Low-Grade Gliomas (Grades 1–2) Slow-growing Less aggressive Often treated with surgery ± chemotherapy Generally favorable prognosis High-Grade Gliomas (Grades 3–4) Rapid growth Highly malignant May arise spontaneously or from lower-grade tumors Require aggressive treatment Glioma Treatment Options Treatment depends on tumor type, grade, and location: Surgery Radiation therapy Chemotherapy High-dose chemotherapy with bone marrow transplant (select cases) Targeted therapy, which attacks cancer cells while sparing healthy tissue Glioma Prognosis (Approximate 5-Year Survival Rates) Grade 1: ~95% Grade 2: ~40–50% Grade 3: ~25–30% Grade 4: ~5–10% Prognosis varies based on individual factors and response to treatment.
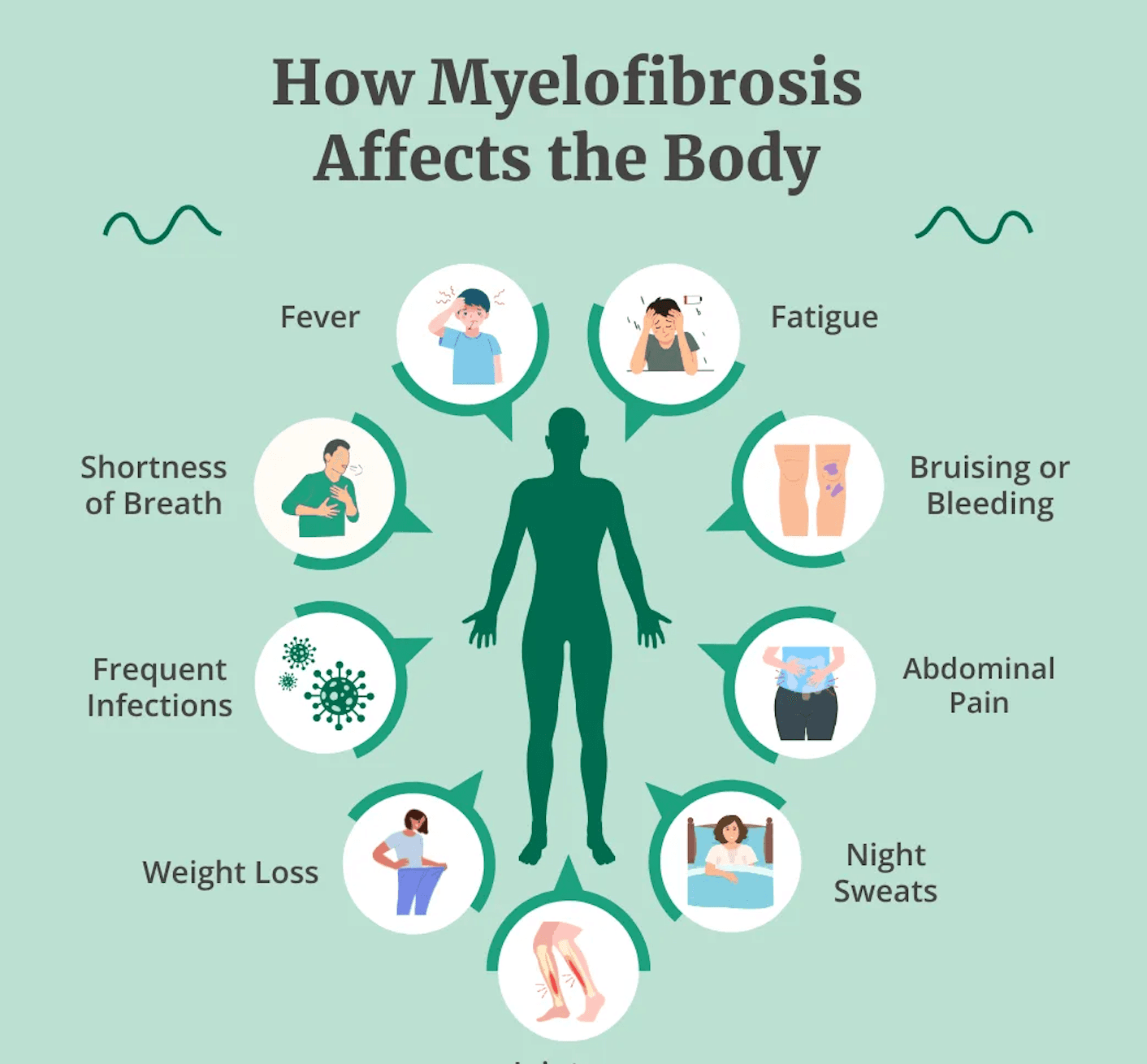
Myelofibrosis (MF)
What Is Myelofibrosis? Myelofibrosis (MF) is a rare type of chronic blood cancer that originates in the bone marrow. In MF, healthy bone marrow tissue is gradually replaced by fibrous scar tissue, a process known as fibrosis. This scarring disrupts the bone marrow’s ability to produce normal blood cells, including red blood cells, white blood cells, and platelets. Myelofibrosis is usually a slow-growing disease, and many people live with it for years without noticeable symptoms. In some cases, however, MF progresses more rapidly and requires timely medical treatment. A hallmark feature of myelofibrosis is the overproduction of megakaryocytes — large bone marrow cells that normally produce platelets. In MF, these cells release excessive amounts of cytokines, proteins that promote inflammation. This chronic inflammation stimulates further scarring in the bone marrow, worsening blood cell production over time. Risk Factors for Myelofibrosis The exact cause of myelofibrosis is not fully understood. However, several factors are associated with an increased risk: Age: Most commonly diagnosed in people over 60 Environmental exposure: Ionizing radiation and petrochemicals such as benzene and toluene JAK2 mutation: Present in approximately 50–60% of MF patients; this mutation causes blood cells to grow and divide abnormally CALR mutation: Found in about 35% of people with MF Other genetic mutations may also play a role, although they are less common. Symptoms of Myelofibrosis Because MF often develops slowly, many patients experience no symptoms in the early stages. As the disease progresses and blood cell production becomes increasingly impaired, symptoms may include: Anemia, leading to fatigue, weakness, and shortness of breath Frequent infections Itching Pale skin Night sweats Fever Unexplained weight loss Abnormal bleeding or easy bruising Bone or joint pain Enlarged spleen (splenomegaly), causing discomfort or a feeling of fullness in the upper left abdomen Enlarged liver Dilated veins in the stomach or esophagus, which may rupture and bleed Portal hypertension, increased blood pressure in the vein connecting the spleen and liver Unexplained blood clots Extramedullary hematopoiesis, where blood-forming cells grow outside the bone marrow, potentially forming masses that compress organs or interfere with their function Types of Myelofibrosis Myelofibrosis is considered a rare form of chronic leukemia and is classified into two main types: Primary myelofibrosis: Occurs on its own, without a prior bone marrow disorder Secondary myelofibrosis: Develops as a complication of another bone marrow disease, such as polycythemia vera or essential thrombocythemia In approximately 12% of primary myelofibrosis cases, the disease can progress to acute myeloid leukemia (AML), a more aggressive and fast-growing cancer.
Get a free consultation
Talk to our experts and discover the best solution for your needs completely free of charge.

Related Articles
Stay informed with our latest medical insights and health tips

Pregnancy and Maternity Care in Switzerland
Switzerland is a top choice for international families seeking maternity care. This guide explains how to plan your birth in Swiss clinics, covering prenatal services, delivery options, postnatal supp...
IVF in Turkey 2026: Best All-Inclusive Packages and Costs
IVF in Turkey offers high success rates, short waiting times, and affordable treatment in certified clinics. Learn what to expect before starting your IVF journey.

Autism Treatment in Georgia
Germany is one of the best countries for autism treatment. Georgia offers advanced autism treatments, experienced clinicians, rapid scheduling, and access to GMP-certified stem cell therapy at competi...
Our doctor is highly skilled and an expert in their field.









